Healthcare organizations must balance patient care with financial stability. One of the most important systems that helps providers maintain consistent revenue is Revenue Cycle Management (RCM). Without an efficient revenue cycle, even busy healthcare practices can struggle with delayed payments, claim denials, and revenue loss.
This guide explains what Revenue Cycle Management is, how it works, and why it plays a critical role in modern healthcare operations.
What Is Revenue Cycle Management?
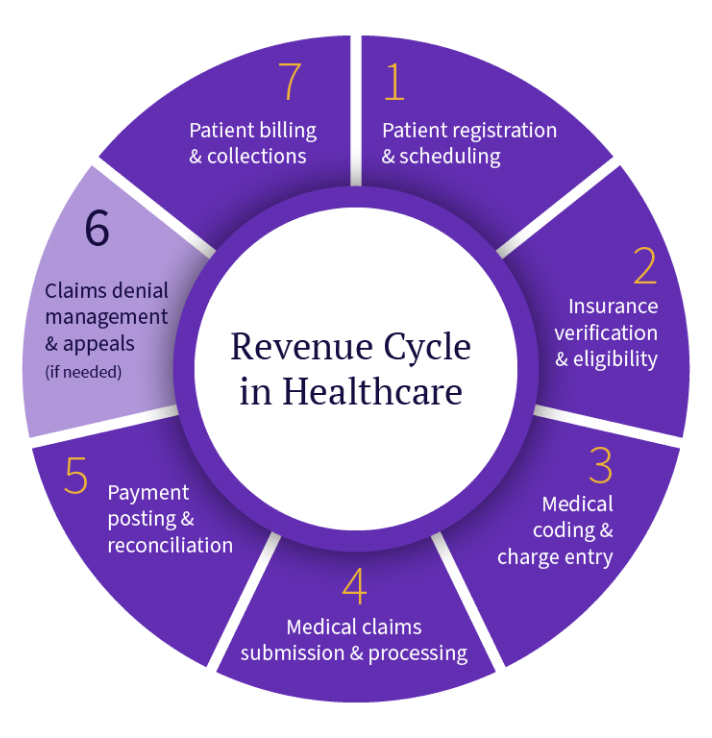
Revenue Cycle Management in healthcare refers to the financial process used to track patient revenue from appointment scheduling to final payment collection. It connects clinical services with billing operations to ensure healthcare providers are properly reimbursed for the care they deliver.
The revenue cycle begins when a patient schedules a visit and ends when all payments — from insurance companies and patients — are received and recorded.
In simple terms, RCM ensures healthcare organizations get paid accurately and on time.
Why Revenue Cycle Management Is Important
Healthcare billing has become increasingly complex due to changing insurance policies, regulatory requirements, and patient payment responsibilities. An effective RCM system helps practices manage these challenges efficiently.
Key Benefits of Revenue Cycle Management
Improves cash flow and financial stability
Reduces claim rejections and denials
Speeds up reimbursement timelines
Enhances billing accuracy
Improves patient financial transparency
Ensures compliance with healthcare regulations
A strong revenue cycle allows providers to focus more on patient care rather than administrative issues.
Revenue Cycle Management involves several interconnected stages:
1. Patient Registration and Scheduling
The process starts when a patient books an appointment. Accurate collection of demographic and insurance information is essential because errors at this stage often cause claim denials later.
2. Insurance Eligibility Verification
Before services are provided, staff verify insurance coverage, benefits, copayments, and authorization requirements. Proper verification reduces payment delays.
3. Medical Coding
Healthcare providers document diagnoses and procedures, which medical coders convert into standardized billing codes such as ICD and CPT codes. Accurate coding ensures compliance and appropriate reimbursement.
4. Charge Capture
All services delivered must be correctly recorded and billed. Missing charges directly result in lost revenue.
5. Claim Submission
Billing teams submit claims electronically to insurance companies. Clean and accurate claims increase first-pass approval rates.
6. Payment Posting
Once insurers process claims, payments are posted into the billing system. This step identifies underpayments and outstanding balances.
7. Denial Management
Denied claims are reviewed, corrected, and resubmitted. Effective denial management helps recover revenue that might otherwise be lost.
8. Accounts Receivable Management
AR teams follow up on unpaid claims and patient balances to reduce aging accounts and maintain steady cash flow.
9. Patient Billing and Collections
Patients receive billing statements for remaining balances. Clear communication improves patient satisfaction and collection rates.
Common Revenue Cycle Management Challenges
Healthcare providers frequently encounter obstacles that affect revenue performance.
Some common RCM challenges include:
High claim denial rates
Incorrect patient information
Coding errors
Slow insurance reimbursements
Manual administrative workflows
Increasing patient payment responsibility
Addressing these issues requires standardized processes and advanced billing technology.
Technology has significantly transformed how healthcare organizations manage revenue cycles.
Modern RCM solutions include:
Automated eligibility verification systems
AI-powered claim scrubbing tools
Electronic health record (EHR) integration
Real-time financial reporting dashboards
Online patient payment portals
Automation reduces manual errors, accelerates billing workflows, and improves overall revenue performance.
Benefits of Outsourcing Revenue Cycle Management
Many healthcare providers choose to outsource RCM services to specialized medical billing companies.
Advantages of Outsourcing
Access to experienced billing professionals
Reduced operational costs
Faster claims processing
Improved compliance management
Better denial prevention strategies
Outsourcing allows physicians and clinical staff to concentrate on delivering quality care instead of managing complex billing tasks.
Best Practices to Improve Revenue Cycle Performance
Healthcare organizations can strengthen their revenue cycle by following proven strategies:
Verify insurance before patient visits
Maintain accurate clinical documentation
Monitor denial trends regularly
Automate billing and follow-up processes
Track key performance indicators (KPIs)
Educate patients about financial responsibility
Continuous monitoring and optimization are essential for long-term financial success.
Conclusion
Revenue Cycle Management is the financial foundation of every healthcare organization. From patient registration to final payment collection, each step directly impacts revenue, operational efficiency, and patient satisfaction.
An optimized RCM process reduces billing errors, accelerates reimbursements, and ensures healthcare providers maintain a healthy cash flow. As healthcare continues to evolve, adopting technology-driven and patient-focused revenue cycle strategies will be essential for sustainable growth.
Effective Revenue Cycle Management ultimately enables providers to do what matters most — deliver exceptional patient care while maintaining strong financial performance.