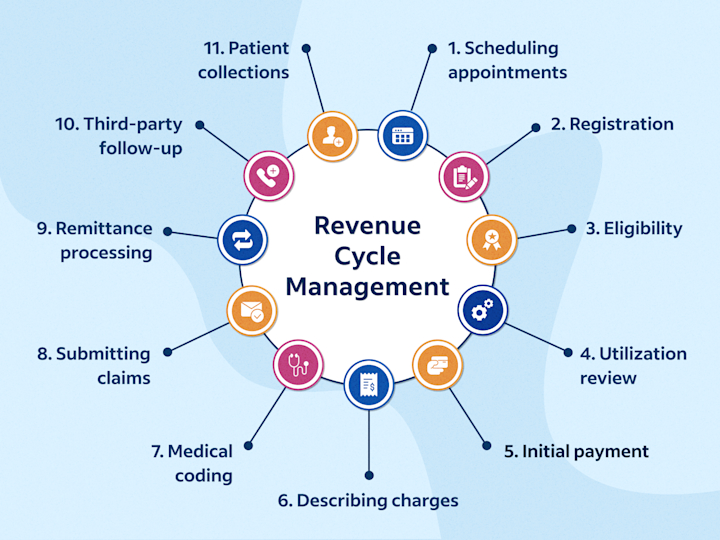
Revenue Cycle Management (RCM) is the financial backbone of every healthcare organization. From patient scheduling to final payment collection, an efficient RCM process ensures steady cash flow, fewer claim denials, and improved operational performance.
However, many healthcare providers struggle with revenue leakage, delayed reimbursements, and administrative inefficiencies. Understanding common Revenue Cycle Management challenges — and implementing the right solutions — is essential for maintaining financial stability and improving patient satisfaction.
This guide explores the most common RCM challenges and practical strategies to overcome them.
What Is Revenue Cycle Management?
Revenue Cycle Management refers to the complete financial process healthcare providers use to manage patient revenue. It includes:
Patient registration
Insurance verification
Medical coding and billing
Claims submission
Payment posting
Denial management
Accounts receivable follow-up
When any step fails, revenue loss occurs. That’s why optimizing each stage is critical.
1. Patient Registration and Eligibility Errors
One of the biggest RCM challenges starts at the front desk.
The Problem
Incorrect patient demographics, outdated insurance information, or missing authorization details often lead to claim denials before billing even begins.
Common issues include:
Wrong insurance IDs
Eligibility not verified
Missing referrals or authorizations
Data entry mistakes
Even small registration errors can delay payments for weeks.
The Solution
Implement real-time insurance verification
Use automated eligibility tools
Train front-desk staff regularly
Standardize intake workflows
Preventing errors at the front end significantly reduces downstream billing problems.
2. Medical Coding Inaccuracies
Medical coding directly impacts reimbursement accuracy.
The Problem
Incorrect CPT, ICD-10, or HCPCS codes can cause:
Claim denials
Underpayments
Compliance risks
Audit exposure
Coding errors often happen due to lack of documentation or outdated coding knowledge.
The Solution
Employ certified medical coders
Conduct regular coding audits
Use AI-assisted coding software
Improve provider documentation practices
Accurate documentation + correct coding = faster reimbursement.
3. High Claim Denial Rates
Claim denials are one of the most costly problems in healthcare revenue cycle operations.
The Problem
Healthcare organizations lose billions annually due to preventable denials caused by:
Missing information
Coding errors
Eligibility issues
Late claim submission
Many practices lack structured denial tracking systems.
The Solution
Establish a denial management workflow
Track denial trends and root causes
Resubmit corrected claims quickly
Implement denial prevention analytics
Top-performing practices focus on denial prevention, not just denial correction.
4. Slow Accounts Receivable (AR) Collections
The Problem
Delayed payments increase AR days and create cash flow instability.
Common causes:
Poor follow-up processes
Aging claims ignored
Inefficient payer communication
Lack of financial accountability
High AR days indicate revenue being trapped in the system.
The Solution
Monitor AR aging reports weekly
Prioritize claims over 30–60 days
Assign dedicated AR follow-up teams
Automate payment reminders and payer follow-ups
Reducing AR days directly improves practice profitability.
5. Inefficient Patient Payment Collection
Healthcare financial responsibility is shifting toward patients due to high-deductible insurance plans.
The Problem
Many practices struggle to collect payments because:
Patients are unaware of costs
No upfront payment policies exist
Limited payment options are offered
Uncollected patient balances significantly affect revenue.
The Solution
Provide transparent cost estimates
Collect copays before visits
Offer online payment portals
Introduce payment plans
A strong patient financial experience improves both revenue and satisfaction.
6. Lack of RCM Technology Integration
The Problem
Disconnected systems between Electronic Health Records (EHR), billing software, and practice management tools create inefficiencies such as:
Duplicate data entry
Billing delays
Reporting inaccuracies
Workflow confusion
Manual processes increase administrative burden and human errors.
The Solution
Integrate EHR and billing platforms
Use automation for claims submission
Implement real-time analytics dashboards
Adopt cloud-based RCM solutions
Technology-driven RCM reduces operational costs and increases efficiency.
7. Compliance and Regulatory Challenges
Healthcare billing regulations constantly evolve.
The Problem
Failure to stay compliant can lead to:
Payment penalties
Claim audits
Legal risks
Revenue loss
Compliance complexity increases administrative pressure on healthcare staff.
The Solution
Conduct compliance training regularly
Stay updated with payer policies
Perform internal audits
Partner with experienced RCM specialists
Compliance-focused workflows protect both revenue and reputation.
8. Limited Revenue Cycle Visibility
Many healthcare organizations lack clear financial insights.
The Problem
Without performance tracking, practices cannot identify revenue gaps.
Typical missing metrics include:
Clean claim rate
First-pass acceptance rate
Denial rate trends
Net collection ratio
The Solution
Implement KPI-based reporting such as:
Revenue dashboards
Predictive analytics
Monthly financial performance reviews
Data-driven decision-making
Visibility transforms reactive billing into proactive revenue management.
Best Practices for Optimizing Revenue Cycle Management
To overcome RCM challenges effectively, healthcare organizations should focus on:
- Front-end accuracy
- Automation and technology adoption
- Continuous staff training
- Data analytics and reporting
- Strong denial prevention strategies
- Patient-centered billing experience
Outsourcing Revenue Cycle Management services can also help practices reduce administrative workload while improving collections and compliance.
Final Thoughts
Revenue Cycle Management challenges are common across hospitals, clinics, and private practices — but they are solvable. Most revenue problems originate from preventable workflow gaps, outdated systems, or lack of process standardization.
By strengthening front-end operations, improving coding accuracy, leveraging technology, and focusing on denial prevention, healthcare providers can build a resilient and profitable revenue cycle.
An optimized RCM process does more than increase revenue — it enhances operational efficiency, reduces staff stress, and ultimately improves patient care outcomes.